|
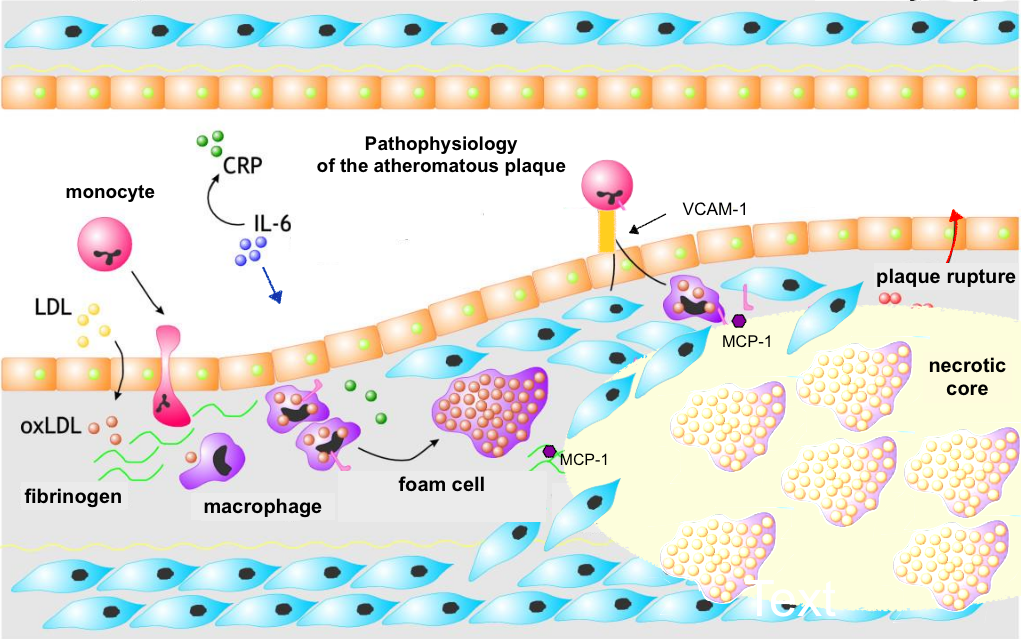
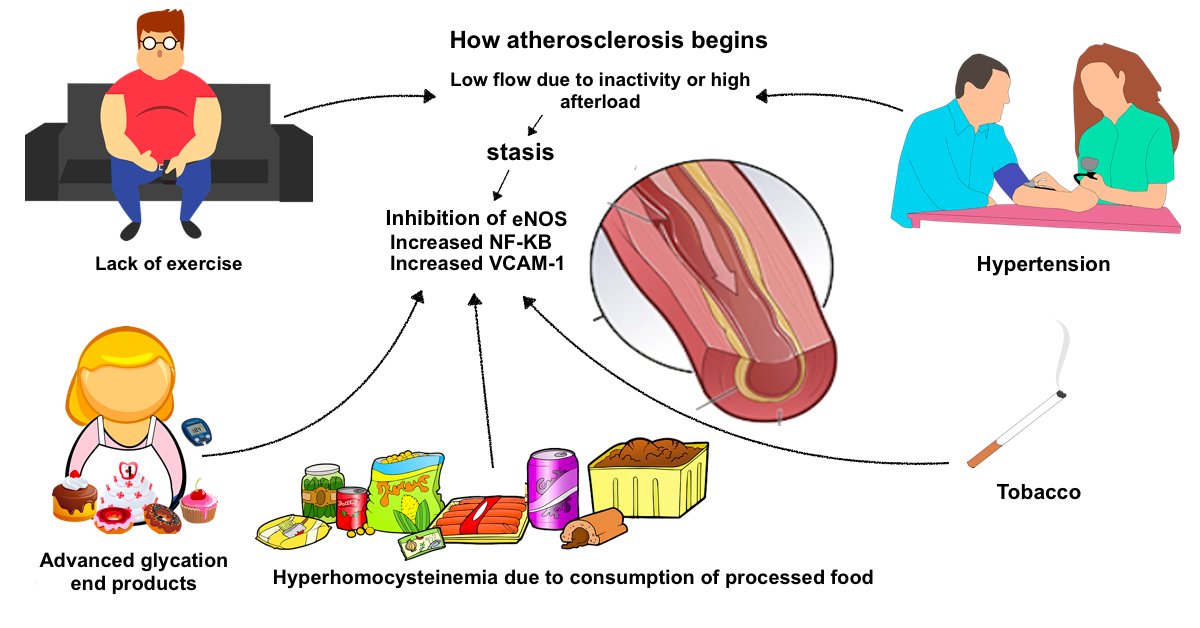
Atherosclerosis begins with an increase in LDL-P levels, that is, an increase in the number of small and dense LDL particles primarily as a result of excess refined carbohydrates (sugar and flour) which stimulate insulin secretion and fructose (juices and sweetened beverages) induced lipogenesis. Smaller LDL particles and VLDL enter the subendothelial space in proportion to their serum level. Apoprotein B of LDL and VLDL interacts with proteoglycans and LDL undergoes oxidation that initiates an inflammatory response. Chronic periodontitis or chronic infections with Chlamydia pneumoniae or Helicobacter pylori activates IL-6 and C-reactive protein and contributes to the inflammatory process. The activation of NF-KB as a signal transducer for atherosclerosis and the inactivation of eNOS (which is the endothelial nitric oxide synthetase that produces nitric oxide) is the result of: -A sedentary lifestyle or hypertension resulting in stasis and decreased shear stress. Atheromatous plaques begin at the bifurcations of the arteries.
-The consumption of refined carbohydrates such as flour and the excesses of fructose from sweetened beverages resulting in an increase in the products of advanced glycation, - Tobacco consumption - The insufficient consumption of fruits and vegetables that results in hyperhomocysteinemia and a deficiency of nitrates and polyphenols in the diet. Inactivation of eNOS results in vasospasm. Activated endothelial cells express monocyte adhesion molecules known as VCAM-1 and chemokine MCP-1. Monocytes bind to VCAM-1 and MCP-1 facilitates the transmigration of monocytes to the subendothelial space. Monocytes are converted into macrophages and express receptors that allow phagocytosis of oxidized LDL cholesterol, VLDL and ApoE residues. The macrophages overflow with lipids and become foam cells. As the space fills with foam cells, they produce chemotactic and proliferative factors that recruit smooth muscle cells that migrate to form a fibrous barrier. If the fibrous layer is firm, the atherosclerotic plaque is stable but at the same time there is less likelihood of regression. If it forms a necrotic center the fibrous layer is more fragile and plaque rupture is more likely .. To see this process in greater detail here is a more extensive summary: Linton MF, Yancy PG, Davies SS, et al. The role of lipids and lipoproteins in atherosclerosis. Endotext
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
August 2018
Categories |

 RSS Feed
RSS Feed